Definition of "Peptic ulcer"
Last modified: less than a minute
Not really. It's basically an ulcer in the stomach. An ulcer is just a break in the mucus lining. The problem is that the tummy is pretty acidic, so it's not as straightforward as an ulcer in the mouth.
Pain, where the break is. The stomach is in the upper part of the tummy, so it'll be painful. The pain is less after eating, because the tummy is less acidic, because it is diluted by food. There can be more burping, even vomiting. You might not feel like eating, and may even lose weight.
The biggie is a particular bacteria, H pylori. NSAID's, although used to reduce pain, have the awful side effect of causing ulceration in the stomach, and therefore, GI bleeds. There are also other things that can contribute to it, like smoking, stress, and disease of the GI and the liver.
Apart from their symptoms, and it getting when you give drugs to decrease stomach acid. You can use a camera down the throat. You can also do an x-ray, but because you can't see the inside of the tummy well because it's soft tissue, you can outline it with contrast, by getting the patient to drink barium. Having said that, if the tummy system has a hole through it, air will escape from the tummy system, into where you usually wouldn't find it. H pylori itself can be detected using a breath test, on biopsy of the tummy, and in the stool.
You can take away things which irritate the tummy's lining, like smoking, NSAID's, alcohol. The biggie is using drugs to decrease stomach acid, which includes PPI's and Histamine-2 blockers. If you know it's H pylori causing the problem, you can also give antibiotics. A camera down the throat might also be needed, if the ulcer is bleeding.
Bleeding is the biggie. Eventually, the full thickness of the tummy's line can also break. This is a massive problem, because stuff in the tummy can leak into the abdominal cavity.
Peptic ulcer [disease] is a break in the lining of the stomach (aka stomach ulcer) [or even the first part of the small intestine (aka duodenal ulcer), or the lower esophagus].
Patient information
What is a peptic ulcer? Has it got anything to do with pepper?Not really. It's basically an ulcer in the stomach. An ulcer is just a break in the mucus lining. The problem is that the tummy is pretty acidic, so it's not as straightforward as an ulcer in the mouth.
Sx
- Upper abdominal pain, causing:
- Waking up at night, due to pain
- Pain improves w/ eating
- Burning or dull aching pain
- Gastric ulcer would give epigastric pain DURING the meal, as gastric acid production is increased as food enters the stomach
- Duodenal ulcers would initially be RELIEVED by a meal, as the pyloric sphincter closes to concentrate the stomach contents, thus acid is not reaching the duodenum. Duodenal ulcer pain would manifest mostly 2-3 hours AFTER the meal, when teh stomach begins to release digested food and acid into the duodenum
- Belching
- Vomiting
- Weight loss
- Poor appetite
- Asymptomatic (33% of older Pt's)
Patient information
What does it feel like to have a break in the lining of the tummy?Pain, where the break is. The stomach is in the upper part of the tummy, so it'll be painful. The pain is less after eating, because the tummy is less acidic, because it is diluted by food. There can be more burping, even vomiting. You might not feel like eating, and may even lose weight.
Causes
- H pylori, bacteria, which increases risk w/ alcohol consumption
- NSAID's, especially sensitive in older Pt's
- Less commonly:
- Tobacco smoking
- Malignancy (gastric cancer)
- Stress due to serious illness
- Crohn disease
- Liver cirrhosis
Patient information
What can cause a break in the stomach's lining?The biggie is a particular bacteria, H pylori. NSAID's, although used to reduce pain, have the awful side effect of causing ulceration in the stomach, and therefore, GI bleeds. There are also other things that can contribute to it, like smoking, stress, and disease of the GI and the liver.
Dx
- Suspected clinically
- Confirmed, if the Sx don't resolve after a few weeks of Tx, or if the Pt>45yo, or has other Sx e.g. weight loss, because stomach cancer can cause similar Sx, w/:
- Endoscopy, esophagogastroduodenoscopy (EGD), to directly visuallly identify, the location and severity of an ulcer
- Barium swallow contrast x-rays
- H pylori can be Dx by:
- Urea breath test, which uses radioactive carbon to detect H pylori. The Pt will drink a tasteless liquid which contains carbon, that the H pylori bacteria breaks down. After 1 hour, the Pt is asked to blow into a bag that is sealed. if the Pt is infected w/ H pylori, the breath sample will contain radioactive CO2. This can thus help monitor response to Tx used to eradicate H pylori
- Culture of a biopsy of the stomach from the EDG, although most labs aren't set up to perform a H pylori culture
- Rapid urease test, to detect urease activity in a biopsy
- Measure antibody levels in blood, although it is controversial, because it is NOT reliable, because of their inability to distinguish between past exposure to bacteria, and current infection. It can also be falsely negative if taking abx, or PPI's
- Stool antigen test
- Histological exam and staining of an EGD biopsy
- CXR, showing "free gas" in the peritoneal cavity. This is because if a peptic ulcer perforates, air will leak from inside the GI tract (which always contains some air) into the peritoneal cavity (which normally NEVER contains air). If the Pt is standing erect for the CXR, the gas will float to a position under the diaphragm
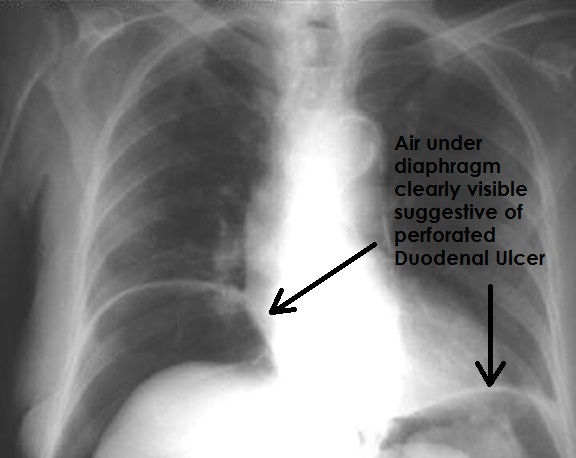
Source: 2010/12/perforated-DU.jpg">Medicalopedia
Patient information
How do you know if someone has a break in the lining of their tummy?Apart from their symptoms, and it getting when you give drugs to decrease stomach acid. You can use a camera down the throat. You can also do an x-ray, but because you can't see the inside of the tummy well because it's soft tissue, you can outline it with contrast, by getting the patient to drink barium. Having said that, if the tummy system has a hole through it, air will escape from the tummy system, into where you usually wouldn't find it. H pylori itself can be detected using a breath test, on biopsy of the tummy, and in the stool.
Tx
- Note that diet does NOT cause or prevent ulcers
- Stop smoking
- Stop NSAID's
- Stop alcohol
- Drugs to decrease stomach acid, w/ 4 weeks of Tx initially recommended, including of:
- PPI's (proton pump inhibitor)
- H2 blocker
- If due to H pylori, add abx Amoxicillin AND Clarithromycin, although as abx resistance is increasing, Tx may not always be effective
- Endoscopy, for bleeding ulcers, or if unsuccessful, open surgery
Patient information
What can you do about a break in the tummy's lining?You can take away things which irritate the tummy's lining, like smoking, NSAID's, alcohol. The biggie is using drugs to decrease stomach acid, which includes PPI's and Histamine-2 blockers. If you know it's H pylori causing the problem, you can also give antibiotics. A camera down the throat might also be needed, if the ulcer is bleeding.
DDx
- Stomach cancer
- Coronary heart disease
- Gastritis (stomach inflammation)
- Cholelithiasis (gallbladder inflammation)
Complications
- GI bleeding (15%), the most common complication. Sudden large bleeding can be life threatening. It occurs when the ulcer erodes one of the blood vessels, e.g. the gastroduodenal artery (i.e. small blood vessel in the abdomen, that supplies blood to the pylorus, that connects the stomach and duodenum)
- GI perforation (perforated ulcer), where an untreated ulcer can burn through the full thickness of the wall of the stomach (or duodenum), allowing digestive juices and food to leach into the abdominal cavity. Perforation at the anterior surface of the stomach causes acute peritonitis, initially chemical, and later bacterial peritonitis. The 1st sign is often sudden intense abdominal pain, an example is Valentino's syndrome (i.e. named after the silent film actor, who experienced this pain before his death). Posterior wall perforation leads to bleeding due to involvement of gastroduodenal artery that lies posterior to the 1st part of the duodenum → can be Dx by erect abdominal/CXR (seeking air under the diaphragm), and Tx requires immediate surgery
- Gastric outlet obstruction
Patient information
What things can happen, due to a break in the stomach's lining?Bleeding is the biggie. Eventually, the full thickness of the tummy's line can also break. This is a massive problem, because stuff in the tummy can leak into the abdominal cavity.
Epidemiology
- Affects 4% of the population at any 1 time, and 10% throughout their life time
- Results in 301k deaths per year, although this number is decreasing
- Incidences of perforated uclers is steadily declining, although it still occurs
See also
- Upper GI bleed
- Perforated ulcer
Synonyms:
Duodenal ulcer
Duodenal ulceration
Gastric ulcer
Gastric ulceration
H pylori
Helicobacter pylori
NSAID induced ulcer
NSAID ulcer
Peptic ulcer disease
Peptic ulceration
Stomach ulcer
Stomach ulceration
Valentino's syndrome
Find a practitioner
Practitioner count: 0
Sponsor a disease. And see how your proceeds help.
$1
Express interest
$10
Write text
$40
Write FAQ
$100
Snap photos
$400
Record audio
$1k
Produce video
$4k
Interview experts