Definition of "Chickenpox"
Last modified: 1 day
Not chickens, but chickpeas, or garbanzo beans. It's because they cause blisters that look like them. It's very contagious, and caused by the varicella zoster virus.
So there are the blisters, that are itchy, and eventualy scab over. They spread over the body. There can also be flu-like symptoms, so fever, fatigue, headache. It's usually worse when it happens in adults.
Chickenpox (aka varicella) is a highly contagious disease caused by initial infection with varicella zoster virus (VZV).
Patient information
What is chickenpox? Anything to do with chickens?Not chickens, but chickpeas, or garbanzo beans. It's because they cause blisters that look like them. It's very contagious, and caused by the varicella zoster virus.
Sx
- Characteristic skin rash that forms small blisters, is itchy, and eventually scabs over
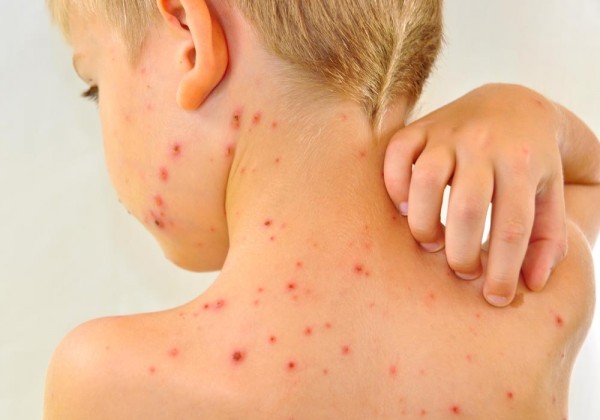
Source: 2013/08/chickenpox-600x420.jpg">Kidspot
- Usually starts on the face, chest, and back; and then spreads to the rest of the body
- Fever
- Fatigue
- Headaches
- Sx usually last 5-10 days
- Disease is more severe in adults than children
- In trimester 3 of pregnancy, an infected mother is more likely to have severe Sx
- Fetal varicella syndrome, presents with:
- Damage ot the brain, including encephalitis, microcephaly, hydrocephaly
- Damage to the eye, including cataracts, optic atrophy
- Neurological disorders, including damage to the cervical and lumbosacral spinal cord, motor/sensory deficits
- Damage to the body, including anal and bladder sphincter dysfunction
- Skin disorders, including skin lesions, hypopigmentation
Patient information
What happens in an infection by varicella zoster virus, that causes chickpea blisters?So there are the blisters, that are itchy, and eventualy scab over. They spread over the body. There can also be flu-like symptoms, so fever, fatigue, headache. It's usually worse when it happens in adults.
And it's super bad when it happens in a pregnant mom?
Yep. Since it can cause fetal varicella syndrome, which can damage the brain, eyes, parts of the body, and skin. Bad stuff.
Pathophysiology
- Varicella zoster virus (VZV, aka chickenpox virus, HHV-3) is 1 of the 8 herpesviruses known to infect humans and vertebrates. It only affects humans, and commonly causes chickenpox in children, teens and young adults and herpes zoster (shingles) in adults and rarely in kids
- VZV multiples in the lungs, and causes a wide variety of Sx
- Airborne disease which spreads easily through coughs and sneezes, of infected persons
- Sx begin 10-21 days after exposure to the virus
- It is infectious from 1-2 days before the rash appears, until all lesions have crusted over
- Pt's with shingles (also caused by VZV) may spread chickenpox to those who aren't immune
- Pt's usually only get chickenpox once
- For pregnant women, antibodies produced due to immunization or previous infection are transferred via the placenta to the fetus → immunized women thus neither need to be concerned for themselves or their infant during pregnancy (and even after delivery, even if other siblings are infected, due to the presence of the mother's antibodies)
- In maternal VZV infection, the varicella infection can spread via the placenta and infect the baby. If it occurs in the first 28 weeks gestation, it can lead to fetal varicella syndrome (aka congenital varicella syndrome)
- Infection late in gestation or immediately following birth is neonatal varicella. The risk is greatest following exposure to infection from 7 days before delivery, up to 8 days following birth
- After the primary infection (chickenpox), the virus goes dormant in the nerves, including the cranial nerve ganglia, dorsal root ganglia, and autonomic ganglia
- Many years after the patient has recovered from chickenpox, VZV can reactivate to cause a number of neurologic conditions
Dx
- Presenting Sx, especially the characteristic rash
- Tzanck smear (aka Tzanck test), scraping of the ulcer base to look for Tzanck cells
- PCR testing, of blister fluid or scabs
- Culturing the fluid, to see if the virus can be grown from a fluid sample
- Blood test, to identify:
- VZV-IgM (acute infection)
- VZV-IgG (previous infection and subsequent immunity) → identify previous chickenpox, thus protection, testing antibodies may be done to determine if a patient is or is not immune
- U/S, for prenatal Dx of fetal varicella infection, although a delay of 5 weeks following primary maternal infection is advised
- PCR (DNA) test of the motehr's amniotic fluid, although there is a risk of miscarriage. Also, having amniocentesis increase the risk of the baby evloping fetal varicella syndrome
Tx
- Varicella vaccine, has resulted in a decrease in the prevalence (has 80% protection), and complications from the disease (protective from more severe disease). Routine immunization is recommended. Immunization even within 3 days of exposure may improve outcomes
- In infants of a mother with perinatal chickenpox:
- Give infant ZIG IM as soon as possible after birth or onset of maternal illness, which must be given within 72 hours. Continue to encourage breastfeeding unless lesions are on or near the nipple
- Give infant IV aciclovir (every 8 hours) in infants who develop chickenpox, didn't receive ZIG prophylaxis within 24 hours, are immunocompromised, or are premature (<28 weeks gestation)
- In postnatal exposure to VZV (<28 days old):
- Give ZIG IM immediately if mother is seronegative, her serology status cannot be determined and Hx is negative, or infant born at <28 weeks gestation or <1kg birth weight
- For itch:
- Calamine lotion to help with itching
- Keeping fingernails short to decrease injury from scratching
- For fever, use of paracetamol
- For those at risk of complications, antivirals (e.g. aciclovir)
Source: VIC Health
Complications
- Pneumonia, especially in newborns
- Encephalitis (brain inflammation)
- Bacterial infections of the skin
- Prematurity delivery, associated w/ maternal infection
Prognosis
- Patients usually only get the disease once
Epidemiology
- Occurs in all parts of the world
- Before routien immunization, the incidence was similar to the number of people born. Since immunizatino, infections have decreased 90%
- Chickenpox resulsts in 7k deaths globally per year. Death occurs in 1 in 60k cases
- Notifiable disease (in those who are vaccinated)
Synonyms:
Chicken pox
Congenital varicella syndrome
Fetal varicella syndrome
HHV 3
Neonatal varicella
Varicella
Varicella zoster virus
VZV
Find a practitioner
Practitioner count: 0
Sponsor a disease. And see how your proceeds help.
$1
Express interest
$10
Write text
$40
Write FAQ
$100
Snap photos
$400
Record audio
$1k
Produce video
$4k
Interview experts